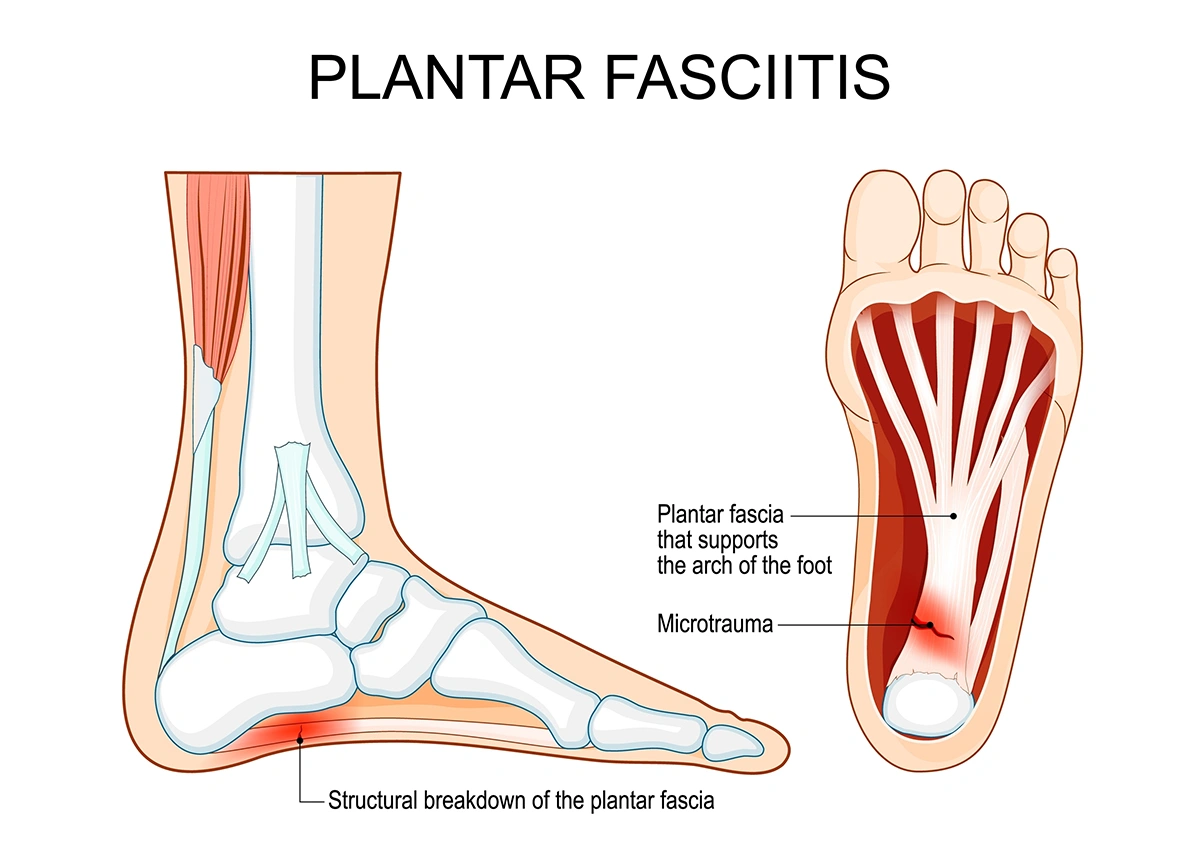
Plantar fasciitis is typically diagnosed through a clinical evaluation, which includes a detailed discussion of symptoms and a physical examination of the foot. The aim is to identify characteristic signs of plantar fasciitis and rule out other possible causes of heel pain.
Medical History
The doctor will begin by asking about your symptoms, including:
- The location of the pain
- When the pain occurs (e.g. first steps in the morning or after rest)
- Activities that worsen or relieve the discomfort
- Any recent changes in physical activity, footwear, or occupation
This information helps determine whether the symptom pattern is consistent with plantar fasciitis.
Physical Examination
During the examination, the doctor may:
- Press on specific areas of the heel and foot to identify points of tenderness
- Assess the arch of the foot and overall foot structure
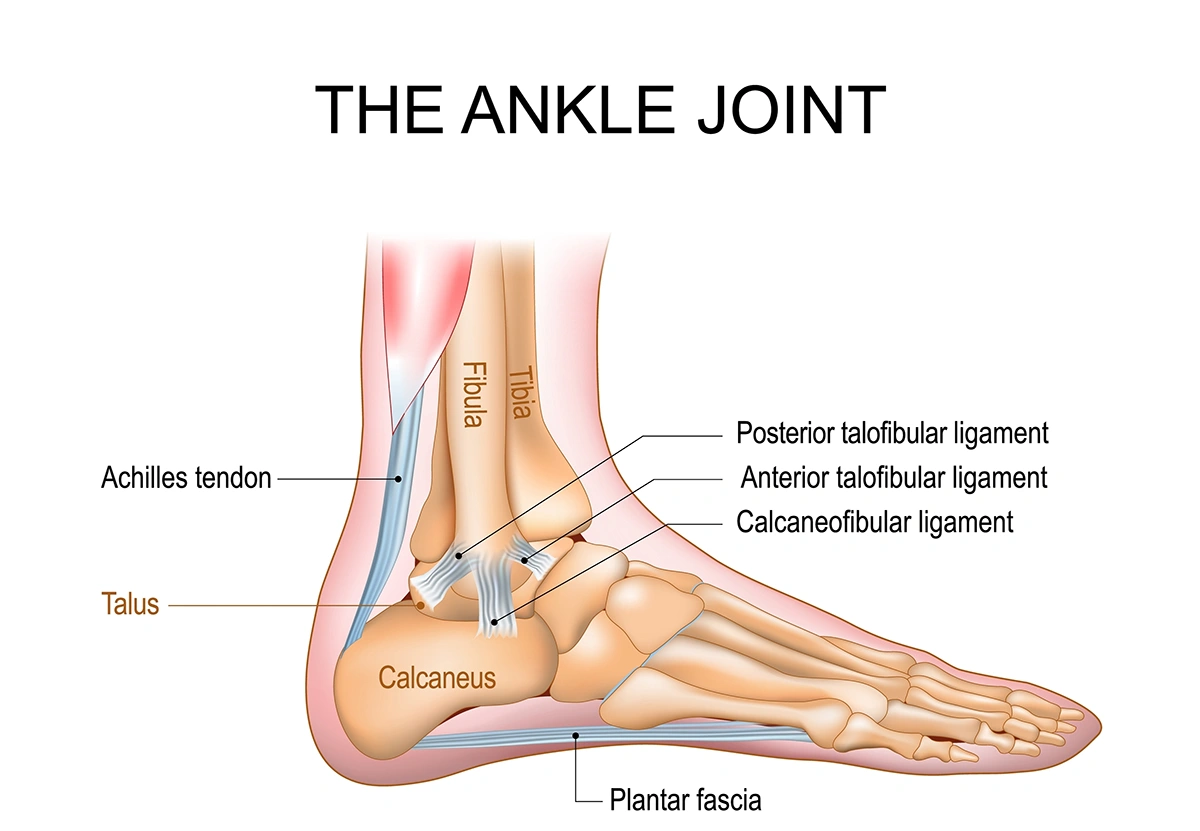
- Check for tightness in the calf muscles or Achilles tendon
- Observe how you stand and walk to evaluate biomechanics
Pain that is localised to the inner (medial) part of the heel is commonly associated with plantar fasciitis.
Imaging Tests (If Required)
In many cases, imaging is not necessary. However, it may be considered if the diagnosis is unclear or if symptoms persist, via:
- X-rays: X-rays may be used to identify the presence of a heel spur or rule out fractures. A heel spur may be seen in some individuals, but does not always correlate with symptoms.
- Ultrasound or MRI: These imaging methods may help assess thickening or changes in the plantar fascia and exclude other conditions such as soft tissue injuries.
Ruling Out Other Conditions
The doctor may also consider other causes of heel pain, such as:
- Stress fractures
- Nerve-related conditions (e.g. tarsal tunnel syndrome)
- Fat pad atrophy
- Inflammatory or systemic conditions